Get A Testing Quote
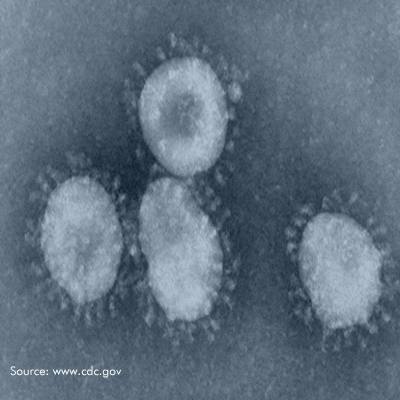
Coronavirus
| Virus | Coronavirus |
| Structure | Enveloped |
| Family | Coronaviridae |
| Host(s) | Humans |
| Disease(s) Caused | Mild to severe respiratory illness |
| Symptoms | Cough, runny/stuffy nose, fever, sore throat, headache, diarrhea |
| Potential Complications |
Pneumonia, death |
| Transmission Mode |
Close person-to-person contact, contaminated fomites |
| Sites of Community Outbreaks | Schools, hospitals, daycare centers |
Importance of Coronaviruses
Two strains of human coronavirus, 229E and OC43, are known to cause approximately 25% of colds that exhibit symptoms similar to those caused by the rhinoviruses (e.g. runny nose, sneezing, and cough). However, recent zoonotic strains of coronavirus characterized by species-jumping from animals to humans have gained notoriety and become of particular concern over the past decade. The SARS-CoV (Severe Acute Respiratory Syndrome coronavirus) outbreak of 2002-2003 originated in bats and spread indirectly to humans via intermediate animals (e.g. civet cats). From the earliest reported cases in southern China, the virus eventually spread to 28 countries over the course of eight months; thousands are believed to have been infected and 774 deaths were reported (1). More recently, the MERS-CoV (Middle East Respiratory Syndrome Coronavirus) outbreak originating in Saudi Arabia in April of 2012 has made headlines due to its high mortality rate of 45% and rapid spread to 9 countries (6); clusters of cases have continued to be reported in the Middle East through the end of 2013.
The Importance of Disinfection: Survival of Coronaviruses on Surfaces and Transmission Potential via Fomites
Having previously crossed species from bats to become endemic in humans (7), coronaviruses 229E and OC43 are spread from person-to-person by way of contaminated aerosols. However, the potential for transmission from contaminated fomites remains of concern as demonstrated by the continued viability of strain 229E more than three hours after drying onto porous and non-porous materials, including aluminum and sterile sponges; strain OC43 remained infectious up to one hour after drying on the same surfaces (11). A comprehensive study evaluating 16 antimicrobial products found that all achieved 3-log10 reductions of human coronavirus strain 229E dried in the presence of organic soil onto stainless steel disks except for a quaternary ammonium compound, a chlorhexidine gluconate-centrimide product, and a phenolic formulation (10). In addition, low levels of sodium hypochlorite, chloramine T, and a mixed halide were not effective, although greater concentrations of these actives did reduce strain 229E levels by 3-log10 (10). No studies have been published to-date detailing disinfection efficacy nor inactivation rates of MERS-CoV on surfaces nor in fluids. Public health agencies such as the CDC recommend the standard disinfection protocols currently in place at hospitals and other patient care centers.
Interestingly, the zoonotic SARS coronavirus strain demonstrated both respiratory and intestinal replication routes for human hosts. A retrospective study of 138 patients infected with SARS-CoV found that almost 40% of patients developed diarrhea, and that SARS-CoV genomic material was detectable in the stool of patients for more than 10 weeks after onset of the initial illness (4). The release of infectious SARS viruses not only into the air, but also into the water supply, further amplified the need for an effective halt to potential environmental transmission. Relative to strain 229E, SARS-CoV maintains infectivity longer in suspension and when dried onto surfaces and is also more thermally resistant (30 minutes at 56 °C and 60 °C) in the presence of 20% fetal calf serum (8). Although SARS-CoV appears to be more environmentally resistant relative to the respiratory coronaviruses, its enveloped structure is still vulnerable to a wide range of disinfectants. Suspension evaluations of propanol (100% and 70%) and ethanol (78%) demonstrated reduction of SARS-CoV to levels below detection in 30 seconds; 60 seconds were required for wine vinegar and 120 seconds for formaldehyde (0.7% and 1%) and 0.5% glutardialdehyde (8). Povidone-iodine (PVP-I) products, quaternary ammonium compounds, free chlorine, and catalytic oxidation via Ag/Al2O3 and Cu/Al2O3 active surfaces have also been proven to completely inactivate SARS-CoV (2, 3, 9, 12). Therefore, environmental transmission of coronaviruses via fomites and liquids can be minimized given the proper implementation of disinfection protocols.
References
- Hawryluck, L., S. Lapinsky, and T. Stewart. 2005. Clinical review: SARS – lessons in disaster management. Critical Care. 9:384-389.
- He, H. et al. 2004. Catalytic inactivation of SARS coronavirus, Escherichia coli and yeast on solid surface. Catalysis Communications. 5: 170-172.
- Kariwa, H., N. Fujii, and I. Takashima. 2004. Inactivation of SARS coronavirus by means of povidone-iodine, physical conditions, and chemical reagents. Japanese Journal of Veterinary Research. 52: 105-112.
- Leung, W. et al. 2003. Enteric involvement of severe acute respiratory syndrome-associated coronavirus infection. Gastroenterology. 125: 1011-1017.
- Mimesh, Z. et al. 2013. Middle East Respiratory Syndrome coronavirus in bats, Saudi Arabia. Emerging Infectious Diseases. 19: 1819-1823.
- Penttinen, P. et al. 2013. Taking stock of the first 133 MERS coronavirus cases globally – is the epidemic changing? Euro Surveillance. 18: 1-5.
- Qian, Z., S. Dominguez, and K. Holmes. 2013. Role of the spike glycoprotein of human Middle East Respiratory Syndrome Coronavirus (MERS-CoV) in virus entry and syncytia formation. PLOS ONE. 8:1-12.
- Rabenau, H. et al. 2005. Stability and inactivation of SARS coronavirus. Medical Microbiology and Immunology. 194: 1-6. Rabenau, H. et al. 2005. Efficacy of various disinfectants against SARS coronavirus. Journal of Hospital Infection. 61: 107-111.
- Sattar, S. et al. 1989. Chemical disinfection of non-porous inanimate surfaces experimentally contaminated with four human pathogenic viruses. Epidemiology and Infection. 102: 496-505.
- Sizun, J, M. Yu, and P. Talbot. 2000. Survival of human coronaviruses 229E and OC43 in suspension and after drying on surfaces: a possible source of hospital-acquired infections. Journal of Hospital Infection. 46: 55-60.
- Wang, X-W., et al. 2005. Study on the resistance of severe acute respiratory syndrome-associated coronavirus. Journal of Virological Methods. 126: 171-177.
Share

