Get A Testing Quote
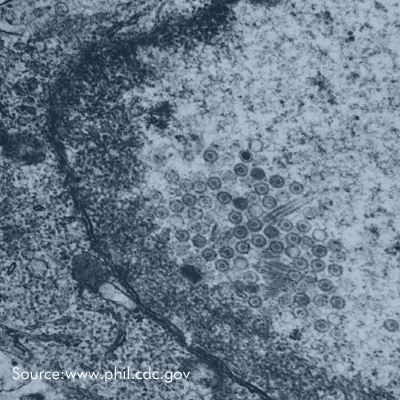
Human Herpesvirus II
| Structure | Enveloped |
| Family | Herpesviridae |
| Disease(s) Caused | Blisters and redness on the genitalia; can also be contracted orally |
| Symptoms | Burning or tingling sensation preceding appearance of blisters: prodrome; Fever, headaches (primary HSV-2 infection) |
| Potential Complications | Herpes simplex encephalitis (newborns); Herpes simplex 2-associated neurological disease |
| Transmission Mode | Person-to-person via intimate contact with mucousal linings of the mouth, vagina, and/or genital skin |
| Natural Reservoirs | Humans |
| High Risk Populations |
Persons w/ multiple intimate partners, persons with a history of STDs |
Importance of Human Herpesvirus II (HSV2)
Herpes simplex virus 2 (HSV-2) – also referred to as human herpes virus-2 (HHV-2) – is the primary cause of genital ulcers in the industrialized world (1). HSV-2 can also infect the mouth, resulting in lesions on the lips and the oral cavity as well, although this occurs less commonly.
Genital herpes is spread most often by intimate contact, and persons who have multiple sexual partners or engage in high-risk sexual activities are particularly at risk for both contracting and disseminating the disease. The first, or primary, outbreak of genital herpes usually occurs within 1 to 2 weeks following sexual exposure. Prodrome of genital herpes is characterized by a burning or tingling sensation in the infected areas, which may include the genitals, anus, buttocks, and/or thighs. In addition, clusters of small, red bumps may appear and develop into blisters. During the next 2 to 3 week period, more blisters can materialize and develop into painful lesions. The lesions will eventually subside and develop scabs or crusts, followed by a relatively rapid period of healing with no visible scarring.
Additional symptoms during primary HSV-2 infection include headaches, fever, and meningitis in some cases. Recurrent HSV-2 outbreaks may follow the primary episode, with a more mild presentation of symptoms including smaller blisters and/or minor itching of the genitalia. Despite the obvious presentation of many cases of HSV-2, it is estimated that ~20% of patients with HSV-2 antibodies are asymptomatic or have lesions in areas that not readily observable (e.g. female cervix) (2). Shedding of infectious HSV-2 virions occurs from lesions by actively infected individuals, as well as from intact skin by asymptomatic persons.
Populations susceptible to complications from HSV-2 infection include persons who are generally immunocompetent, as the nature of infection following the primary episode is marked by recurrent outbreaks (average of 4 to 5 annually) that may be marked by significant morbidity and psychological distress. Patients that are immunocompromised (e.g. cancer patients and transplant recipients) can experience a highly severe form of primary herpes characterized by extensive, widespread lesions. Most severely infected, however, are newborns; exposure to HSV-2 during vaginal birthing may result in permanent neurological damage even when antiviral therapies are instituted immediately after birth or upon presentation of symptoms.
The Importance of Disinfection: Survival of Human Herpesvirus II (HSV2) on Surfaces and Transmission Potential via Fomites
Like herpes simplex-1, HSV-2 is an enveloped virus that spreads primarily by direct contact with the infected skin and/or secretions of carriers. It may remain infectious on dry, inanimate surfaces for up to seven days (4), which raises the issue for potential transfer to human skin. The likelihood of this transmission route is very low for the average individual, although it can not be ruled out for individuals engaging in high risk sexual behaviors.
The potential for transmission via contaminated objects may be lessened by antiseptic agents formulated for use on inanimate surfaces. Several commercially-available products applied to HSV-2 at diluted concentrations reduced infectious viruses to levels below detection. Bleach (2,000 ppm) and 70% isopropanol (1 part virus stock:1 part alcohol) also demonstrated complete inactivation of HSV-2 after 10 minutes and at time zero, respectively (3).
References
- Ashley, R.L. And A. Wald. 1999. Genital herpes: review of the epidemic and potential use of type-specific serology. Clinical Microbiology Reviews. 12: 1-8.
- Corey, L. 1994. The current trend in genital herpes. Progress in prevention. Sexually Transmitted Diseases. 21 (Supplement 2): S38-S44.
- Croughan, W.S. and A.M. Behbehani. 1988. Comparative study of inactivation of herpes simplex virus types 1 and 2 by commonly used antiseptic agents. Journal of Clinical Microbiology. 26: 213-215.
- Kramer, A., I. Schwebke, and G. Kampf. 2006. How long do nosocomial pathogens persist on inanimate surfaces? A systematic review. 6:130.
Share

