Virucidal Efficacy Testing
Get A Testing Quote
In the United States, virucidal disinfectants used on environmental surfaces are regulated by the Environmental Protection Agency (EPA) under the Federal Insecticide, Fungicide, and Rodenticide Act (FIFRA).
The Environmental Protection Agency (EPA) regulates disinfectants as antimicrobial pesticides. In order for a disinfectant to be sold in the United States, it must undergo registration with both the EPA and the applicable state authority where it will be sold. Currently, the U.S. EPA does not recognize “virucidal sanitizers” – all virucides must meet disinfectant-grade efficacy guidelines.
To register a virucidal disinfectant, companies must submit chemical characterization, safety, and efficacy data to the EPA, as well as pay registration fees. Efficacy data should be generated in compliance with Good Laboratory Practice Regulations (GLP). Test methods used should be taken from the Series 810 guidance, and companies should consult the EPA’s Pesticide Registration Manual.
Virucidal Efficacy Testing Is Different – Here’s How:
Disinfectant Testing Basics:
The EPA currently only recognizes “hard surface carrier” methods for substantiation of virucidal efficacy claims. These methods consist of a non-porous carrier (typically glass) being inoculated with the selected virus, dried, and then treated with the disinfectant. Virucidal hard surface carrier methods are quantitative, meaning that percent and log reductions are calculated by determining the TCID50 (50% Tissue Culture Infective Dose) per carrier before and after treatment with the disinfectant. The disinfectant must demonstrate complete inactivation of the virus down to the limit of detection of the assay, or (if cytotoxicity is observed) a ≥ 3.00 log10 reduction (99.9%).
Observation of Results:
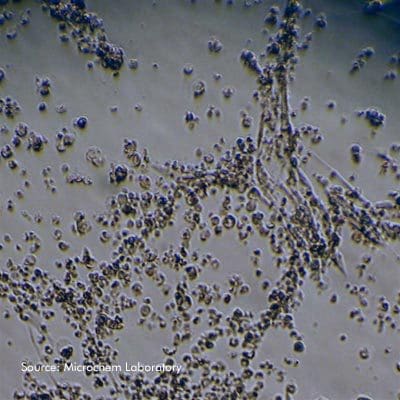
Virus testing is unique within the laboratory because the presence of viruses before and after product treatment is not determined by observing growth of virus but rather by observing the damage caused by infection to mammalian host cells. When virologists analyze individual sets of cells after a study, they use a microscope to look for where healthy cell layers become damaged. This damage is known as the cytopathic effects (CPE) of infection. The quantity and quality of CPE is used to calculate the amount of virus present.
CPE is typically observed as changes to cell appearance and monolayer (the layer host cells form when they attach to a flask or tray) disruptions. CPE can vary depending on the virus and host cell line used. Some instances of CPE are distinct, consisting of severe monolayer disruption and cell rounding. Some CPE can be subtle, consisting of gradual enlargement of host cells that is only recognizable when compared to a negative control. In cases where CPE is difficult to distinguish, special confirmatory assays are used to verify the results of the assay. Some more common confirmatory assays include Hemagglutination Assays (HA) and immunofluorescent staining (IF).
Study Preparation and Timeline:
From the laboratory’s perspective, a significant amount of work and time is required to grow and maintain the sterile cell cultures that are needed to propagate and detect viruses in antimicrobial efficacy studies. From our customer’s point of view, the cell culture requirement means that extra time must be given to the laboratory to prepare for and execute the study. Most studies take 1-2 weeks to complete, though some can take 3-4 weeks. The behind-the-scenes cell culture work and extraordinary expertise necessary to conduct virological assays also means that virological studies are more expensive than their related bacteriological assays.
Host Cell Line and Stock Virus Preparation:

- Host Cell Line Preparation:
- Flasks are seeded with the host cell line and incubated until a monolayer is formed. This can take about 5-7 days depending on the cell line.
- After the incubation period, the cell line is seeded into 24 well plates in preparation for testing at its idea growth conditions and incubated until the appropriate confluency is achieved (~70-80%).
- Stock Virus:
- The virus is propagated by inoculating the appropriate cells in the appropriately sized flask. The virus and cells are incubated anywhere from 6 hours to 7 days to allow the virus to enter the cell and multiply
- After the incubation period, the flask goes through a series of freeze-thaw cycles that burst the cells and release the virus inside.
- The virus is extracted, aliquoted into cryovials, and placed in a deep freeze. This stock virus is ready to use in testing.
- The virus titration is also performed at this point to observe the number of infective units
Study Conduct and Parameters:
There are two main viral morphologies – enveloped and non-enveloped. Non-enveloped viruses consist of genetic material surrounded by a hard protein coat. Enveloped viruses have an additional lipid layer encompassing their protein coat. The limited sensitivity of non-enveloped viral components means that these viruses can persist in an infectious state even when exposed to harsh environmental conditions – including exposure to UV or relatively high temperatures. When it comes to testing, this means that one can translate almost any bacteriological study into a non-enveloped viral assay without changing too many parameters.
Enveloped viruses are another story. Their delicate lipid envelopes leave them vulnerable to environmental factors like osmotic pressure, low humidity, and high temperatures. When working with enveloped viruses, certain parameters (like contact times and contact temperatures) and even general study methods may need to be modified to accommodate the unique demands of these microbes.
Viruses Tested at the Laboratory*
- Adenovirus 1
- Adenovirus 2
- Bovine Viral Diarrhea Virus (US EPA-Approved Hepatitis C Surrogate)
- Bovine Rotavirus
- Canine Distemper Virus
- Canine Parainfluenza Virus
- Canine parvovirus
- Coronavirus (human)
- Coxsackievirus B3
- Coxsackievirus B6
- Echovirus 11
- Enterovirus 68
- Enterovirus 71
- Epizootic Hemorrhagic Disease Virus
- Equine Herpesvirus 1
- Feline Calicivirus (US EPA-Approved Norovirus Surrogate)
- Human herpesvirus 1 (HSV1)
- Human herpesvirus 2 (HSV2)
- Human herpesvirus 5 (Cytomegalovirus)
- Hepatitis A virus
- Influenza A virus, H1N1 (human)
- Influenza A virus, H1N1 (swine)
- Influenza B virus
- Measles virus
- Minute Virus of Mice
- MS2 Bacteriophage (Viral Screening Tool)
- Poliovirus 1
- Respiratory Syncytial virus (RSV)
- Rhinovirus
- Rotavirus (Group A)
- Vesicular Stomatitis Virus
- Zika Virus
* Microchem Laboratory is happy to acquire additional viruses to meet your testing needs. Contact us today to discuss viral acquisition and your testing options.
Virucidal Efficacy Test Methods and Services
Preliminary Testing and Guidance
- Preliminary Screening (MS2 Bacteriophage)
- Initial and Confirmatory Virucidal Effectiveness Testing for Viral Surrogates
Suspension-Based Tests
- ASTM E1052 – Standard Test Method for Efficacy of Antimicrobial Agents Against Viruses in Suspension
- EN 14476 – Chemical Disinfectants and Antiseptics – Quantitiative Suspension Test for the Evaluation of Virucidal Activity in the Medical Area (Phase 2/Step 1)
Hard Surface Carrier Tests
- ASTM E1053 – Standard Test Method to Assess Virucidal Activity of Chemicals Intended for Disinfection of Inanimate, Nonporous Environmental Surfaces
- AOAC Germicidal Spray Test, Modified for Viruses
- Pre-Saturated Towelettes Virucidal Effectiveness Test
Treated Surfaces and Textiles
- AATCC 100 – Assessment of Antibacterial Finishes on Textile Materials, Modified for Viruses
- JIS Z 2801 – Measurement of Antimicrobial Activity of Plastic Surfaces
- ISO 22196 – Test for Antimicrobial Activity of Treated Surfaces
- EPA Copper Sanitization
- Modified ISO 21702 – Measurement of Antiviral Activity on Plastics and Other Non-porous Surfaces
Additional Testing
- Custom Virucidal Efficacy Studies – UV/Room Device/Antimicrobial Devices
- Disinfectant Validation Studies Against Viruses
- Residual Self-Disinfection
Share!